-
Recent Posts
Archives
- October 2022
- August 2022
- May 2022
- March 2022
- January 2022
- December 2021
- September 2021
- July 2021
- June 2021
- May 2021
- April 2021
- February 2021
- January 2021
- November 2020
- October 2020
- September 2020
- June 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- June 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- January 2017
- December 2016
- November 2016
- August 2016
- July 2016
- June 2016
- May 2016
- April 2016
- March 2016
- February 2016
- January 2016
- December 2015
- November 2015
- October 2015
- September 2015
- August 2015
- July 2015
- June 2015
- May 2015
- April 2015
- March 2015
- December 2014
- June 2014
- May 2014
- April 2014
- November 2013
- September 2013
- August 2013
- July 2013
- June 2013
- May 2013
- March 2013
- January 2013
- November 2012
- October 2012
- July 2012
- December 2011
- November 2011
- October 2011
- September 2011
- August 2011
- July 2011
- June 2011
- May 2011
- April 2011
- March 2011
- February 2011
- January 2011
- December 2010
- November 2010
Categories
Cool Case Maggie
 Maggie, a 10-year-old Yorkshire Terrier, presented to NorthStar VETS for acute respiratory distress and cyanosis (turning blue), noticed by the pet-sitter while the owners were returning home from vacation. She had a history of tracheal collapse, but before this episode, she had been doing pretty well. Upon arrival, she had a honking cough and was significantly dyspneic (trouble breathing). She was successfully stabilized by the Emergency team with oxygen therapy and sedation.
Maggie, a 10-year-old Yorkshire Terrier, presented to NorthStar VETS for acute respiratory distress and cyanosis (turning blue), noticed by the pet-sitter while the owners were returning home from vacation. She had a history of tracheal collapse, but before this episode, she had been doing pretty well. Upon arrival, she had a honking cough and was significantly dyspneic (trouble breathing). She was successfully stabilized by the Emergency team with oxygen therapy and sedation.
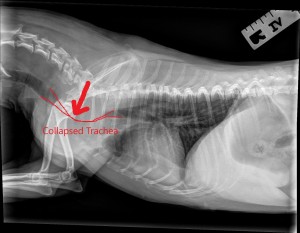 Chest X-rays revealed severe collapse of her cervical trachea (as seen in the image). We gave her a few days of attempted medical management; however, she continued to have very noisy breathing, coughing and episodes of cyanosis when taken out of the oxygen cage. Because of the severity of the collapse and her episode, it was elected to manage her condition with a tracheal stent placement.
Chest X-rays revealed severe collapse of her cervical trachea (as seen in the image). We gave her a few days of attempted medical management; however, she continued to have very noisy breathing, coughing and episodes of cyanosis when taken out of the oxygen cage. Because of the severity of the collapse and her episode, it was elected to manage her condition with a tracheal stent placement.
Tracheal collapse is a condition from cartilage weakness in the trachea that causes the normally open, “C-shaped” cartilage rings to collapse down partially or completely. When this happens, it causes a honking cough and does not allow air to normally pass through it. It is an irreversible and progressive condition common in small-breed dogs, especially Yorkies like Maggie.
It can be managed medically or surgically. Medical management involves cough suppressants, anti-histamines, intermittent steroids, keeping the dogs trim and using harnesses, not collars. In most cases, we can successfully manage their clinical signs and coughing with these treatment options. When the case is more severe, or if it causes life-threatening signs, as in Maggie’s case, we opt for a procedural intervention. This is done by placing a nitinol, meshwork stent inside the tracheal lumen to give it support and keep it open. It does not eliminate the cough completely, but usually improves it significantly and prevents the life-threatening respiratory episodes.
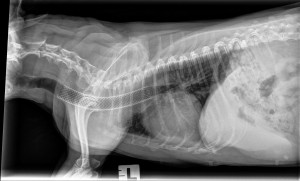 Understanding the risks of this respiratory procedure, Maggie’s owners decided to move forward with the stent placement. She was placed under general anesthesia and the size of the stent was chosen based on measurements taken via fluoroscopy. The endotracheal tube (tube used to delivery oxygen and anesthetic gas) was removed and the stent was deployed in her trachea covering the collapse area and keeping it nice and open (as seen in the image).
Understanding the risks of this respiratory procedure, Maggie’s owners decided to move forward with the stent placement. She was placed under general anesthesia and the size of the stent was chosen based on measurements taken via fluoroscopy. The endotracheal tube (tube used to delivery oxygen and anesthetic gas) was removed and the stent was deployed in her trachea covering the collapse area and keeping it nice and open (as seen in the image).
She recovered beautifully, and for the first time since we met her, she was able to breathe quietly and be with us outside of the oxygen cage. She was immediately happy, alert and wanting to eat! It was truly a night-and-day difference.
Maggie went home the next day breathing normally. Months later, Maggie is at home and doing extremely well. She coughs occasionally, which is expected for dogs with tracheal stents, but it is minimal and has not led to any further respiratory distress episodes. We love hearing how well she is doing at home and that she is enjoying time with her family!
Learn more about the Interventional Radiology service at NorthStar VETS.
Melanie Puchot, DVM, DACVIM
 Dr. Melanie Puchot is a Texas native who received her veterinary degree from Texas A&M University College of Veterinary Medicine in 2013. After graduation, she completed a small animal rotating internship at Cornell University in Ithaca, NY. She then returned to Texas A&M University and completed a 3-year residency in small animal internal medicine in 2017. She has a special interest in endocrinology, nephrology and interventional endoscopy / radiology. Dr. Puchot is excited to join the team at NorthStar VETS.
Dr. Melanie Puchot is a Texas native who received her veterinary degree from Texas A&M University College of Veterinary Medicine in 2013. After graduation, she completed a small animal rotating internship at Cornell University in Ithaca, NY. She then returned to Texas A&M University and completed a 3-year residency in small animal internal medicine in 2017. She has a special interest in endocrinology, nephrology and interventional endoscopy / radiology. Dr. Puchot is excited to join the team at NorthStar VETS.
The information presented on this web site is not intended to take the place of your family veterinarian’s advice and is not intended to diagnose, treat, cure or prevent any disease. Discuss this information with your own veterinarian to determine what is right for your pet. All information is intended for your general knowledge only and is not a substitute for medical advice or treatment for specific medical conditions. We can not and do not give you medical advice via this blog. The information contained in this online site and emails is presented in summary form only and intended to provide broad understanding and knowledge. The information should not be considered complete and should not be used in place of a visit, call, consultation or advice of your veterinarian. We do not recommend the self-management of your pet’s health problems.
This entry was posted in Pets, Veterinary Medicine and tagged Melanie Puchot DVM, NorthStar VETS, tracheal stent, Veterinary Internal Medicine, veterinary surgery. Bookmark the permalink.





Leave a Reply