-
Recent Posts
Archives
- October 2022
- August 2022
- May 2022
- March 2022
- January 2022
- December 2021
- September 2021
- July 2021
- June 2021
- May 2021
- April 2021
- February 2021
- January 2021
- November 2020
- October 2020
- September 2020
- June 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- June 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- January 2017
- December 2016
- November 2016
- August 2016
- July 2016
- June 2016
- May 2016
- April 2016
- March 2016
- February 2016
- January 2016
- December 2015
- November 2015
- October 2015
- September 2015
- August 2015
- July 2015
- June 2015
- May 2015
- April 2015
- March 2015
- December 2014
- June 2014
- May 2014
- April 2014
- November 2013
- September 2013
- August 2013
- July 2013
- June 2013
- May 2013
- March 2013
- January 2013
- November 2012
- October 2012
- July 2012
- December 2011
- November 2011
- October 2011
- September 2011
- August 2011
- July 2011
- June 2011
- May 2011
- April 2011
- March 2011
- February 2011
- January 2011
- December 2010
- November 2010
Categories
Hemodialysis for Pets
Yes, it’s true. Dogs and cats are able to benefit from hemodialysis just as people are. The use of hemodialysis in veterinary medicine is a little different compared to people but the basic principles are the same. Here we will explain the basics of hemodialysis as well as the indications for this treatment in dogs and cats.
What is the normal function of the kidney?
The kidneys (there are usually two – left and right) are organs located in the abdomen. Their primary job is to filter the blood, removing by-products of metabolism and toxins from the body. Kidneys also participate in the following:
- Keeping blood electrolyte and mineral concentrations in the normal range
- Red blood cell production
- Blood pressure control
- Regulation of water content in the body
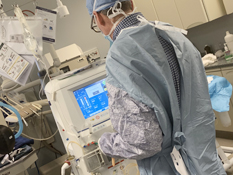 What is hemodialysis?
What is hemodialysis?
Hemodialysis is the movement of blood through a filter and cleaning the blood of toxins that build up in the body when the kidneys are not working effectively. The filter is located outside of the body and the blood is moved through a blood circuit.
Is a special catheter used?
The use of a hemodialysis catheter facilitates the movement of blood outside of the body. This catheter is larger than regular intravenous catheters allowing high flow rates of blood. In most pets, placement of the hemodialysis catheter is in the right jugular vein. A majority of dogs and cats will have placement of the catheter under general anesthesia. X-rays confirm proper placement of the catheter. Sterility is of utmost importance to reduce the risk of infection. The hemodialysis doctors place these catheters with the same sterility as a surgeon uses when performing surgery.
Why would my pet need hemodialysis?
Many of us have had a family member or friend treated with hemodialysis, or have seen movies or TV programs showing people getting hemodialysis. Hemodialysis conjures an image of people living the rest of their life hooked up to a machine. In this situation, these people have end-stage kidney disease caused by chronic illness such as diabetes or high blood pressure. As these people have no hope of regaining normal kidney function, they will remain dependent on hemodialysis for the remainder of their lives. Some people may be candidates for a transplant but for most, hemodialysis (or chronic peritoneal dialysis) remains the only option.
In veterinary medicine, cost and considerations of quality of life for pets limit the use of hemodialysis for treatment of chronic kidney disease. Most often, veterinarians use hemodialysis to treat acute kidney disease. Acute kidney disease differs from chronic kidney disease for many reasons. Of these differences, reversibility of the underlying process is the most important, especially when we are recommending hemodialysis to treat a patient with acute kidney disease. Long-standing damage to the kidney leading to loss of the normal kidney function of filtering the blood leads to illness. Various diseases can lead to chronic damage of the kidney tissue. In response to this damage, scar tissue builds up, leading to irreversible loss of kidney function. These chronically damaged kidneys have little to no ability to repair themselves.
Acute kidney disease differs in that there is a chance of repair and return to normal function. Acute insults to the kidney can lead to acute kidney injury. The insult could be an infection (e.g. leptospirosis), a toxin (e.g. ethylene glycol, non-steroidal anti-inflammatory drugs), and/or decreased blood flow, to name a few. Once damaged, the kidney’s function declines and the pet starts to feel sick. Treatment of the underlying disease can eliminate the ongoing damage. The kidney then has a chance at repairing itself and function returning to normal or near normal. Repair of the organ tissue can take days to months, leaving the kidney function abnormal during that time. Many patients with acute kidney damage will respond to supportive care and treatment of the underlying disease and there is no need for hemodialysis. These treatments may include intravenous fluids, antibiotics, and anti-vomiting medications. When the degree of damage is enough to cause marked accumulations of toxins in the body and/or the loss of the ability to make urine, and supportive treatments are not leading to improvement of kidney function, hemodialysis is a treatment consideration.
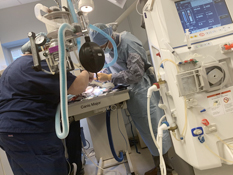 If my pet needs hemodialysis, how long does treatment last?
If my pet needs hemodialysis, how long does treatment last?
Hemodialysis does not fix the kidneys. It merely filters the toxins from the blood, making the pet feel better and allowing their kidneys time to heal. The speed at which the kidneys heal vary and depend on the underlying cause as well as variations between individual pets. In the beginning, a pet may need daily treatments. When the patient stabilizes, treatments may be every 2-3 days. When kidney function is improved or the patient is making urine, dialysis ceases and traditional medical treatments continue until the patient goes home. Kidney recovery can take between 2-6 weeks (sometimes months) and patients may need dialysis treatments for 2-4 weeks. In some cases, we can treat pets on an outpatient basis, having them come in every 2 days for treatment. We find most patients only need dialysis for the first 1-2 weeks.
Individual treatment sessions last between 4-12 hours depending in the cause of the kidney dysfunction. Treatment times depend on a number of factors. The initial treatments typically last the longest and become shorter during the course of hospitalization.
How will my pet receive nutrition during treatments?
Most patients with kidney injury or disease will have poor appetites, and as nutrition is very important, many pets will have a feeding tube placed at the time of the hemodialysis catheter placement. An esophagostomy tube is commonly used. Placement of the esophagostomy tube occurs with the patient under general anesthesia. The advantage of an esophagostomy tube is that we can feed a complete, balanced diet that promotes recovery.
Can hemodialysis treat diseases other than kidney disease?
The answer is a resounding, YES! Removal of toxins from the blood can occur with the combined techniques of hemodialysis and hemoperfusion. Hemoperfusion utilizes a special charcoal filter that binds toxins, removing them from the blood. Hemoperfusion has been used successfully to treat toxicities in both dogs and cats.
What is the prognosis?
The prognosis for recovery from acute kidney damage in dogs and cats treated with hemodialysis depends on the cause, extent of renal damage, concurrent disease, and presence of multiple organ system involvement. Based on the published studies, global survival for dogs with severe acute uremia is approximately 50 percent. Survival from infectious (60 percent), hemodynamic and metabolic etiologies (40 percent) was greater than survival from toxic causes (20 percent). The outcome for dogs with acute leptospirosis is especially favorable with 80-90 percent survival with either severe (dialysis-dependent) or milder forms (medically manageable) of acute renal failure (ARF). Reported global survival for cats requiring hemodialysis is 56 percent. Overall, hemodialysis substantially increases the global survival for both dogs and cats with severe acute kidney damage beyond what would be expected with conventional management.
What about chronic kidney disease?
Dogs and cats with chronic kidney disease can undergo long-term hemodialysis. This is similar to people who get hemodialysis 3 times a week for the remainder of their lives. Veterinary patients can experience a very good quality of life. Patients have been treated chronically and still go hiking with their human companions and live amazing lives. We must remember, however, that this is a huge commitment, from an emotional and financial point of view. Not all pets are good candidates. A hemodialysis doctor will perform a detailed review of the case and they will determine if your pet is a candidate for chronic hemodialysis.
Summary
Hemodialysis can be a life-saving procedure for patients with acute kidney injury, allowing patients greater chance of survival. For patients with a treatable underlying disease, hemodialysis is a reasonable consideration for any pet experiencing severe acute kidney disease.
Learn more about Hemodialysis at NorthStar VETS.
Benjamin Davidson, BVSc, MANZCVSc, DACVECC
 Dr. Davidson graduated from the University of Queensland School of Veterinary Science in 1998. He obtained experience as an emergency veterinarian for five years before starting a residency in small animal emergency and critical care at the Cummings School of Veterinary Medicine at Tufts University in 2003. He completed his residency in 2006 and became board certified in emergency and critical care the same year. Dr. Davidson then took on a role as a senior clinician at BluePearl Veterinary Partners in New York City, where he headed the critical care service for ten years. He then headed the critical care and hemodialysis services at BluePearl in Paramus, NJ. Board certified and proficient in all fields of veterinary emergency and critical care, Dr. Davidson’s professional interests include mechanical ventilation, trauma, sepsis and extracorporeal methods of organ support, including hemodialysis, ultrafiltration and membrane oxygenation. Dr. Davidson has authored articles and textbook chapters on the topics of critical care, and routinely lectures to veterinarians.
Dr. Davidson graduated from the University of Queensland School of Veterinary Science in 1998. He obtained experience as an emergency veterinarian for five years before starting a residency in small animal emergency and critical care at the Cummings School of Veterinary Medicine at Tufts University in 2003. He completed his residency in 2006 and became board certified in emergency and critical care the same year. Dr. Davidson then took on a role as a senior clinician at BluePearl Veterinary Partners in New York City, where he headed the critical care service for ten years. He then headed the critical care and hemodialysis services at BluePearl in Paramus, NJ. Board certified and proficient in all fields of veterinary emergency and critical care, Dr. Davidson’s professional interests include mechanical ventilation, trauma, sepsis and extracorporeal methods of organ support, including hemodialysis, ultrafiltration and membrane oxygenation. Dr. Davidson has authored articles and textbook chapters on the topics of critical care, and routinely lectures to veterinarians.
The information presented on this web site is not intended to take the place of your family veterinarian’s advice and is not intended to diagnose, treat, cure or prevent any disease. Discuss this information with your own veterinarian to determine what is right for your pet. All information is intended for your general knowledge only and is not a substitute for medical advice or treatment for specific medical conditions. We can not and do not give you medical advice via this blog. The information contained in this online site and emails is presented in summary form only and intended to provide broad understanding and knowledge. The information should not be considered complete and should not be used in place of a visit, call, consultation or advice of your veterinarian. We do not recommend the self-management of your pet’s health problems.
This entry was posted in Pets, Veterinary Medicine and tagged acute kidney injury, Benjamin Davidson, hemodialysis, NorthStar VETS. Bookmark the permalink.





Leave a Reply